Big Sick or Little Sick - A rapid approach to casualty assessment and critical decision making
A core philosophy of all of our courses from basic one-day introductory courses to more advanced Pre-Hospital Care training is the concept of “Big Sick or Little Sick?” A rapid approach to casualty assessment and critical decision making.
Whilst seemingly basic, almost childish, this model is used for our initial assessment and decision making whether you are a novice First Aider or a Consultant Anaesthetist. Any casualty can be assessed as Big Sick (critically ill or injured) or Little Sick (not critically ill or injured) by simply asking ”Is it normal?”
In this article we will look at how we can rapidly assess a casualty's state of health, at a basic level, with no reliance on medical terminology, equipment or numbers using their Vital Signs
The common mistake
Humans are genetically hardwired to react to the sight of blood and generally make their initial judgement on casualties based on their injury.
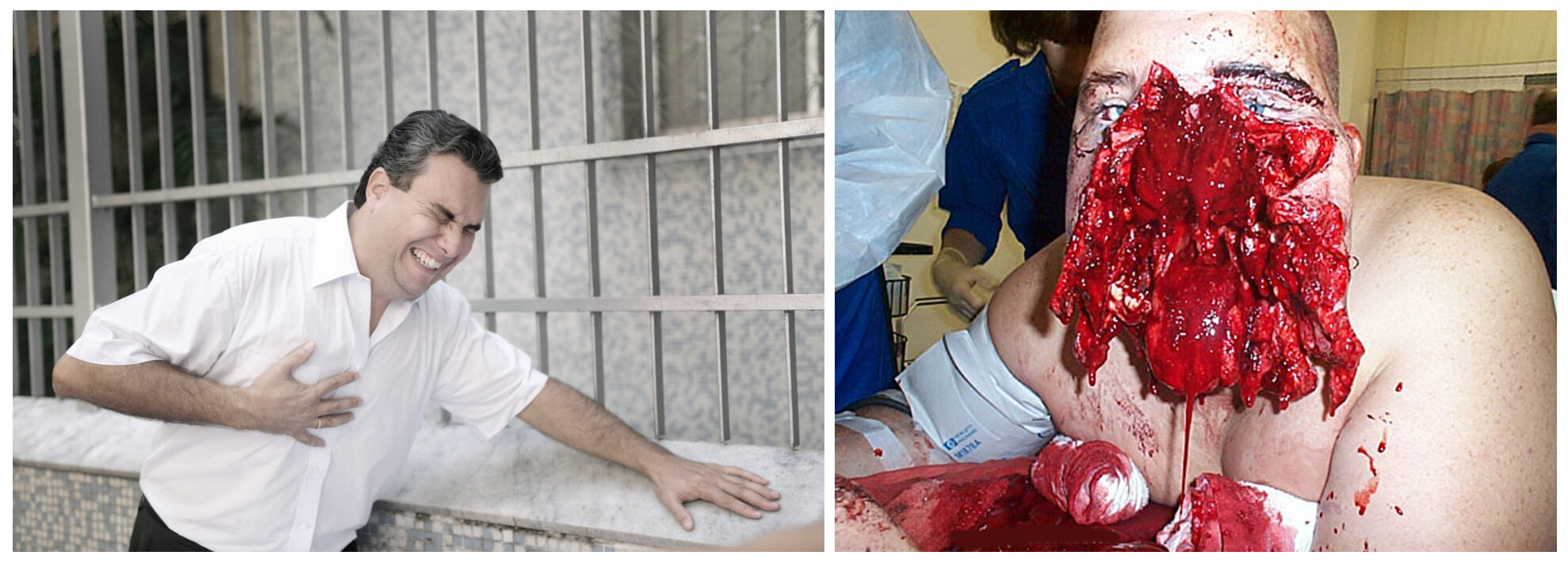
For example, which would you say are Big Sick or Little Sick?
Most people would gauge the injuries on the right as more severe - Big Sick - and the injuries on the left as minor - Little Sick. Some injuries can be more serious than others but injuries alone do not necessarily tell you if the casualty is Big Sick or Little Sick - will the live or will they die? Injuries alone cannot necessarily tell you if a person is going to live or die or if so, when. Injuries can only tell you that someone has an injury.
If we look at the two casualties below, which casualty is Big Sick?
Most people’s automatic response is to assume the casualty on the right is Big Sick based on the severity of his injury. Despite having a serious injury there is nothing in this photo which suggests they are going to die any time soon. Whilst they ahve a serious injury, they are, in fact, Little Sick. The casualty on the left is far less distracting. Despite the absence of any blood, the suggestion of chest pain, pale colour, probable difficulty breathing suggests he is Big Sick. In simple terms the casualty casualty on the left is likely to die quicker than the casualty on the right.
This is is an important rule - while we judge injuries based on the amount of blood, the bruising or the shape of the limb, we cannot do the same with casualties:
Some injuries can look horrific but be relatively minor. Superficial head injuries can bleed a lot despite the wound being very small and will easily stop bleeding with direct pressure.
Some casualties may have no injuries whatsoever but their condition can be life threatening.
How do we judge a casualty who has no visible injury but they tell you the feel 'unwell'? How do we judge a casualty who is unconscious or uncommunicative?
The answer is to assess their 5 Basic Vital Signs.
Level of Response
When dealing with a casualty, one of the first questions you will be asked by either an emergency services call handler or the person stood next you is "Are they conscious?"
This is a closed question. When we are asked “Are they conscious?” we only ever answer with "Yes" or "No".
Consciousness is a spectrum: We want to know the casualty’s Level of Response (LoR)
If you are reading this you are more than conscious, you are fully ALERT - and that is different to simply being conscious: Someone who is fully ALERT:
Is oriented in place and time - they know where they are and what is going on around them.
Can speak clearly
Can give appropriate answers
If your casualty is not ALERT, are they unconscious? Possibly. Despite the common use of the term ‘unconscious’ in First Aid, the term is rarely used in medicine, rather unresponsive. But we can also have casualties, who are not fully alert and not classically unconscious which leads to vague terms such as ‘semi-conscious’ (which should be avoided at all costs).
Unconsciousness is not like turning off a switch; there are various shades of unconsciousness. They may appear ‘unconscious’ but they may also still be able to respond to stimuli.
Typically on approach, we ask the unconscious casualty "Are you OK?" or "Can you hear me?" These again are closed questions which, firstly, can only ever be answered with “Yes” and secondly only yield very simple responses.
Start by asking the casualty an open questions such as "Tell me what happened."
If the casualty appears unconscious but is able to say "I've fallen over, I've really hurt my back" even though they may appear unconscious they are in fact ALERT. They know where they are, what has happened and they are speaking clearly and appropriately.
If the reply is mumbled or slurred words, they are not Alert, therefore they are described as RESPONSIVE TO VOICE.
If they don't reply to questioning, shout a strong and simple command like "Open your eyes!"
The response you get may be overt - they may actually open their eyes and look at you - or their response may be subtle, they may simply groan or flinch. In either case, whilst they may appear unconscious, this casualty is still RESPONSIVE TO VOICE
If they do not respond to voice, do they respond to pain? It is at this point on First Aid courses we traditionally tell people to pinch the casualty's ear lobe, which is entirely ineffective. Unfortunately, to ascertain if your casualty is able to respond to pain, you must administer genuine pain - BUT - it must be appropriate. There are various techniques including pinching the trapezius, applying a sternum rub or rubbing a knuckle into the sternocleidomastoid. This is our prefer technique:
Hold the casualty’s head still with both hands on either side of the face. This can be done from the head or kneeling next to the casualty. This prevents unwanted movement if the casualty is able to respond to pain.
With your index fingers, find the angle of the jaw on either side.
Press inwards, into the muscle with both fingers behind the jaw. Applying pain to both sides also reduces unwanted movement of the neck compared to applying pain to one side of the neck or shoulder.
Look at the casualty's face; any response is a response, be it overt (e.g. eyes open and screaming) or it may be subtle ( a grimace or a flinch).
This casualty is RESPONSIVE TO PAIN
(Obviously, if your casualty is responding to voice, do not check to see if they respond to pain!)
If they do not respond to pain, they are UNRESPONSIVE.
Your casualty can now be categorised using AVPU:
"Alert" or
"Responding to Voice" or
"Responding to Pain" or
“Unresponsive”
REMEMBER: You do not want to know IF they are unconscious, you want to know HOW RESPONSIVE they are.
This is one of the most complex ideas for us to get our head around. If you were to ask anyone what an unconscious casualty looks like, most people would say "laying down", “not moving” and "eyes closed". Neither of these are anything to do with being unconscious....
What about the drunk, staggering around the town centre at 2am, hugging lamp posts and singing to the moon: He is upright, his eyes are open. Is he conscious?
A better question is 'Is he ALERT?' Does he know where he is? Does he know what time it is? Can he give you an appropriate answer? Is he speaking clearly?
No. So he must be....Unconscious?
When you shout over to him "Hey! Are you alright?" And he swings around, almost loosing balance, all he has done is responded to your voice.
This casualty is upright with his eyes open described as RESPONDING TO VOICE.
If your casualty is not ALERT, that is not normal. That is bad. This casualty is potentially Big Sick
Common causes for unconsciousness include:
A Alcohol / Altitude /Allergies
E Epilepsy / Environment (heat stroke or hypothermia)
I Insulin (too much or too little)
O Overdose (medication or drugs)
U Underdose (medication)
T Trauma
I Infection (Sepsis)
P Poisoning
S Stroke
Breathing
In the same way that people tend to simply ask 'Are they conscious?' people will also ask 'Are they breathing?' This is also a Yes/No question. Knowing if someone is breathing simply tells you they are alive. Knowing if someone is not breathing simply tells you they are dead. It does not tell you if they are Big Sick or Little Sick. You do not want to know IF they are breathing, you want to know HOW they are breathing.
RATE - Is it too fast or too slow? Forget the numbers initial, does it seem normal?
EFFORT - Breathing should require no effort.
DEPTH - How much air is moving? Is it shallow / light / weak or is it deep / heavy / strong?
RHYTHM - Is it irregular?
NOISE - Breathing should be silent. Are they Wheezing? Gurgling? Rasping?
None of these are normal. All of these are bad. Anyone whose breathing is not normally is Big Sick.
Colour
Skin colour is another obvious, intuitive Vital Sign; we all judge - consciously or not - an individual's skin colour; we will notice when someone looks pale or flushed. We can tell which one of the passengers is looking sea sick!
Most changes to skin colour are intuitive:
Pale - Blood is moving away from the skin, typically to the core, to protect us when we are cold loosing blood or short of oxygen.
Blue - If the cold, blood loss or lack of oxygen is not resolved, we eventually go blue, at the extremities first (peripheral cyanosis) followed by blueness around the mouth and eyelids (central cyanosis). This is not normal. This is Bad!
Red - blood is moving towards the skin, usually to help us cool. If the person has a history of exercise and is in a hot climate this would be normal. This would be little sick. If the casualty is sat at their desk in an air conditioned office but is hot and red, this is not normal, this is bad. This is Big Sick.
Yellow - Jaundice, for example, can have an effect of skin colour due to a build up of bilirubin which stains the blood an orangey colour, which appears yellow through the skin.
Green - Do people go green? Who knows, but you can quite accurately tell when someone is going to be sick just by the look of them.
Ethnicity
Changes in skin colour are most noticeable in Caucasian skin because the skin is contains less pigmentation making it almost translucent, a bit like grease proof paper (if you have ever peeled off the flap of skin left over from a blister). We are able to see blood through the skin and how it is changing - whether it is moving close to the surface, further away or if there is a stain to it.
In casualties with strong ethnicities, this becomes more difficult as the greater amount of pigmentation in the skin masks the changes we would otherwise see.
Whilst it can be difficult to notice changes in skin colour when dealing with people of different ethnicities, it is not impossible:
We are all pale in the same places; everyone has pink conjunctiva (behind the lower eyelid) and finger nails which will go pale or blue.
Colour is closely associated with temperate - blue is cold, red is hot. This is a universal.
Jaundice will also reveal itself in staining the sclera, the 'white' of the eye.
While it can be harder to notice abnormal skin colours in strangers because you do not have a normal baseline reference, we are able to notice changes in the skin colour of people we know because, regardless of ethnicity, we know what normal is for them.
Temperature
Casting you're mind back to when you were a little boy or little girl, you Mum would usually measure your temperature by feeling your forehead with her hand. And we know that Mums are always right.
If your casualty feels hot, they are hot. If your casualty feels cold, they are cold. All we have to ask is "Is it normal?"
Is it normal for:
The environmental temperature
Their levels of activity
Their clothing
This is simple enough for an initial assessment.
For long term monitoring you will need a thermometer. If the casualty is getting cold/hot due to the environment, your hands will be getting cold/hot. Checking the casualty's temperature every 5 minutes you will have forgotten what it felt like last time you checked.
The most accurate thermometers are tympanic (ear) thermometers but they are bulk and expensive; ideal for parents at home not ideal for remote or industrial first aid kits. Infra-red forehead thermometers are smaller and cheaper. Digital Fridge thermometers are tiny and dirt cheap. These are also ideal for monitoring a packaged casualty.
Tympanic Thermometer
Infra-red Forehead Thermometer
Digital Fridge Thermometer
Monitoring a casualty's temperature is essential for managing the casualty with infection, illness, heat stroke or hypothermia.
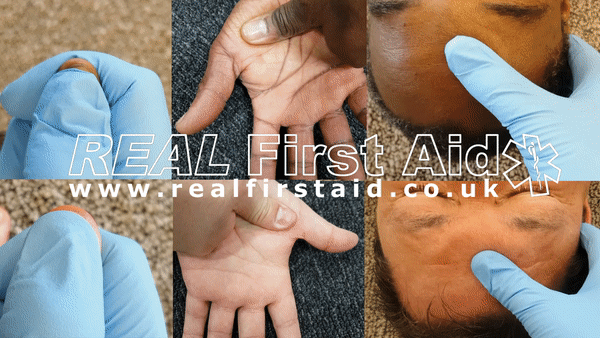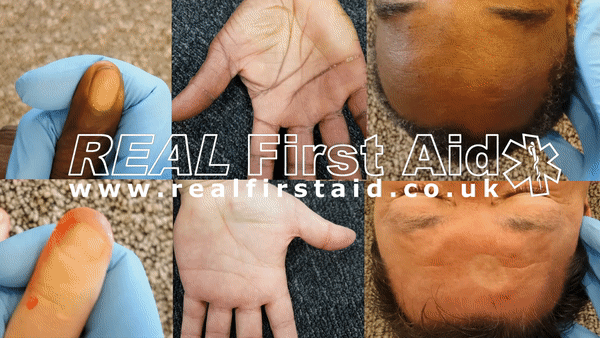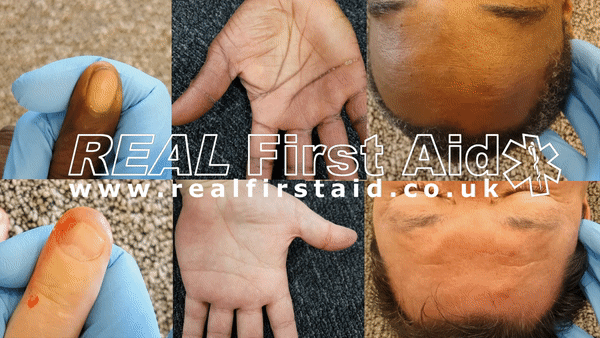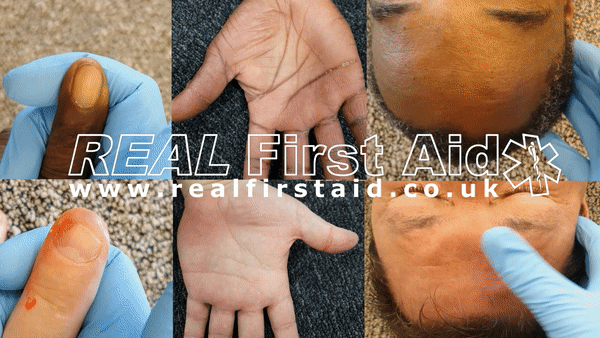
Capillary Refill
Taking a pulse manually is time consuming, requires regular practice and rarely accurate. A quicker, easier and more reliable test is Capillary Refill.
Pressing on the casualty's forehead or sternum for 5 seconds will push blood from that area. When you remove your thumb the pale patch you have created will refill with blood as colour returns. This should happen within 2 seconds. Capillary Refill only happens if the casualty has enough circulating blood.
If the casualty does not have enough blood they will be pale and the pale patch will not be apparent. This could indicate hypovolaemic shock.
If the casualty does not have circulating blood, the pale patch will take longer to refill, if at all.
If the colour refills almost instantaneously, there is too much peripheral perfusion, vasodilation is sending blood to the skin which could indicate head injury, anaphlayxis or sepsis.
Exceptions
Capillary Refill does not work on non-Caucasian skin. In this instance test for capillary refill on the casualty's finger nail:
Expect the refill to take longer than 2 seconds.
Capillary Refill at the finger nail is affected by the cold more than the forehead.
Example
Watch the short clip below and ask yourself, is the casualty Big Sick or Little Sick?
Is the casualty Alert? No, they are only responding to voice, and that's not normal, that's bad.
Is the casualty Breathing? Yes. But it's not normal, that's bad.
They look pale. That is not normal, that is bad.
This is what differentiates Big Sick from Little Sick; because the casualty's Vital Signs aren't normal, that's bad, this casualty is Big Sick. We don't necessarily know what is wrong with the casualty at this stage but we know he is Big Sick.
For the casualty in the clip above it would be reasonable for a lay-person to respond in the following way:
Call Handler: "Are they conscious?"
You: "Yes."
Call Handler: "Are they breathing?"
You: "Yes."
So what have you just told the person you are requesting help from? They are conscious and breathing. Are they at all concerned?
Better replies would be:
Call Handler: "Are they conscious?"
You: "No, but they are responding to Voice."
Call Handler: "Are they breathing?"
You: "Yes, but it is deep and noisy. He is also quite pale”
These descriptors inform the person you are contacting that the Vital Signs are not normal and with this information, professional help will begin to form an opinion of what could be wrong with the casualty.
An experienced emergency services call handler will continue to ask more probing questions but we cannot guarantee that everyone we contact will have that ability. If we are relaying information to the Emergency Services via a 'runner' we need to ensure the runner can answer these questions appropriately.
BIg Sick or Little Sick in other situations
The concept of Big Sick / Little Sick is robust enough to apply to all casualties by looking for normal responses.
Hypothermia
It is normal to shiver when we are cold so a cold casualty who is shivering is Little Sick. They are able to regulate their own temperature. A casualty who is cold and not shivering is not normal. That’s bad. They are Big Sick. They are no longer to look after themselves.
Heat Illness
It is normal to sweat when we are hot so someone who is hot and sweaty is Little Sick. They have enough fluids and are currently attempting to regulate their own temperature. A casualty who is very hot and bone dry is not normal. That’s bad. They are Big Sick.
Epilepsy
It is normal for a casualty with epilepsy to have a seizure. It is also normal for most seizures to be less than five minutes. If a casualty with known epilepsy has a seizure of less than five minutes, and regains consciousness in less than five minutes afterwards, and fully recovered, that is normal. They are Little Sick. If a casualty with known epilepsy has a seizure of more than five minutes, remains unconscious for more than five minutes after that or has a series of seizures, that is not normal. That’s bad. They are Big Sick.
Head Injury
It is normal for a casualty who has sustained a head injury to go unconscious, it is a natural response. It is also normal for that unconsciousness to last less than 5 minutes. If they have lost consciousness for less than five minutes, that is normal. They are Little Sick. They will go to hospital as soon as possible by which ever means are convenient. If they remain unconscious for more than five minutes, that’s not normal. That’s bad. They are Big Sick and warrant immediate transfer to hospital via the emergency services.
CSM
If an injured limb has normal circulation, sensation and movement at the end, that is Little Sick. It may be a nasty injury but there is no vasuclar or neurological compromise so it is not time critical, it is Little Sick. If the limb does not have normal circulation, sensation or movement below the injury, that’s not normal, that’s bad. That injur is time critical and Big Sick.
Summary
It is the Vital Signs that tell us if the casualty is Big Sick or Little Sick and all we have to ask is "Are they normal?"
The 5 basic Vital Signs are
Level of Response
Breathing
Colour
Temperature
Capillary Refill
A casualty may have horrific injuries but if they are Alert, breathing normally, with normal skin colour and at a normal temperature, they are Little Sick. They are not going to die any time soon. A nd that is reassuring because while the injuries may be disturbing we know we have plenty of time.
A casualty may have no injuries at all but if they have a reduced level of consciousness, their breathing is not normal, their skin colour has changed or they are not a normal temperature, they are Big Sick. And this is important because it prompts us to act even though there is no obvious injury.
If we monitor the Vital Signs over time we will notice changes. This may reveal if the casualty is improving, deteriorating or stable.
We would love to say this was an original concept but it was taught to us in the early days of Remote First Aid in the UK, 20 years ago by Pete Harvey of Wilderness Expertise. Pete brought it back to the UK in the late 90’s from his Wilderness EMT training in the US at the National Outdoor Leadership School who first pioneered this idea in the 1980s.
Thank you Pete and NOLS.